Weekend update
From Capitol Hill, the House of Representatives and the Senate will be engaged in Committee business and floor voting this week. Bloomberg brings us up to date on the status of $3.5 trillion budget reconciliation bill which the President and Democrat leaders in Congress have been pushing.
From the Delta variant front, it must be recalled that before health plans become obligated to cover the mRNA booster for immunized folks over age 65 and a broader group of immuno-compromised Americans, fifteen days must pass from the time that the Centers for Disease Control ratifies the FDA’s decision from last Friday. The CDC’s Advisory Committee on Immunization Practice is scheduled to consider this issue on September 29. The press reports on Friday indicated that the CDC is expected to establish the scope of the expanded coverage of immuno-compromised Americans.
On Sunday’s talk shows, Drs. Fauci and Collins, according to the Wall Street Journal, predict that the FDA will approve the mRNA booster for the general population before long. Kaiser Health News discusses how these leading scientists got in front of their skis on the scope of the mRNA booster coverage issue.
Precision Vaccines discusses where Britain and American stand in terms of achieving at least limited herd immunity.
In the USA, new data from the U.S. CDC published by the JAMA Network on September 2, 2021, indicates herd immunity may be achievable soon.
This review is based on blood donations in the U.S. from July 2020 through May 2021, including both natural infection- and vaccine-induced SARS-CoV-2 seroprevalence. This repeated cross-sectional study included over 1.4 million blood donation specimens representing 74% of the US population.
The estimated SARS-CoV-2 seroprevalence weighted for differences between the study sample and general population increased from 3.5% in July 2020 to 20.2% for infection-induced antibodies and 83.3% for combined infection- and vaccine-induced antibodies in May 2021.
The coronavirus seroprevalence differed by age, race, ethnicity, and geographic region of residence, and these differences changed over the course of the study.
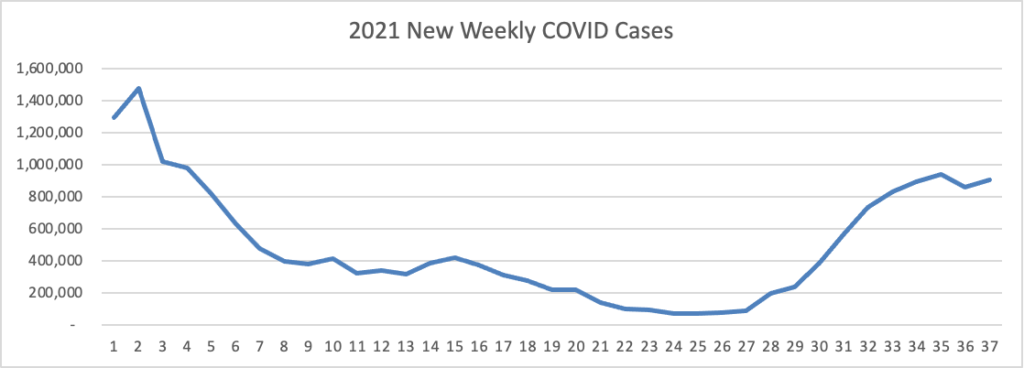
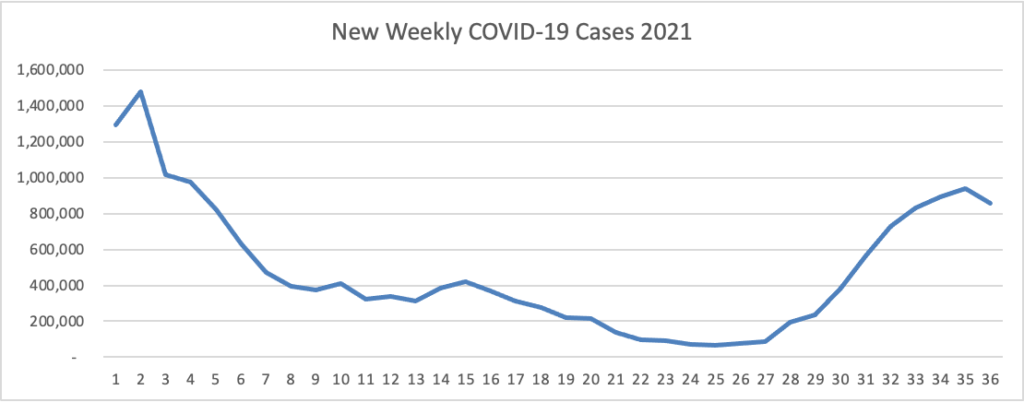
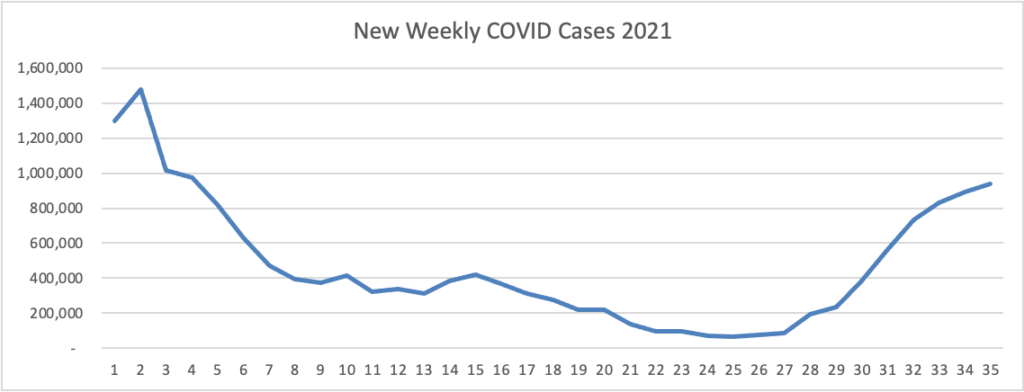
Since May 2021, the U.S. CDC has reported significant increases in COVID-19 vaccinations, initial infections, and re-infections. More than 4 million of these cases have been reported in the past few weeks.
These new totals may soon push the USA over the 95% herd immunity goal.
It’s worth noting that Britain is ahead of the U.S. because the Delta variant struck Britain first.
In other updates —
- The American Cancer Society has released the 2021 edition of Cancer Facts and Figures.
- The American Medical Association provides background of the 2022 changes to the Current Procedure Terminology. The AMA publishes the CPT which is one of the code sets for HIPAA electronic transactions.
- Fierce Healthcare reports “The Biden administration has delayed enforcement of payer-to-payer data exchange included in a May 2020 final interoperability rule until future regulations are finalized.” The interoperability rules apply to insurers with HHS contracts, not FEHB carriers.
- Health Payer Intelligence informs us that “Healthcare B2B payment transactions have been high in 2021, potentially signaling the importance of electronic payment transfers as the nation emerges from the coronavirus pandemic, according to a report from National Automated Clearing House Association (NACHA).” What’s more “‘This data from Nacha is good news for payers, providers and members,’ said April Todd, senior vice president of CORE and explorations at CAQH. ‘The increase in electronic payment volume likely indicates that people who deferred routine medical appointments due to COVID are now able to get the care they need. And when that care is paid electronically, it is more efficient and cost-effective for the industry.’ Todd’s organization has been tracking the economic impact of transitioning to electronic payment. A CAQH report estimated that the healthcare industry could see $426 million in cost savings by transitioning to electronic payments. Switching to electronic payment for claims submissions could save providers around $2 for each claim. Exact savings can vary based on the type of transaction.”