Friday Stats and More
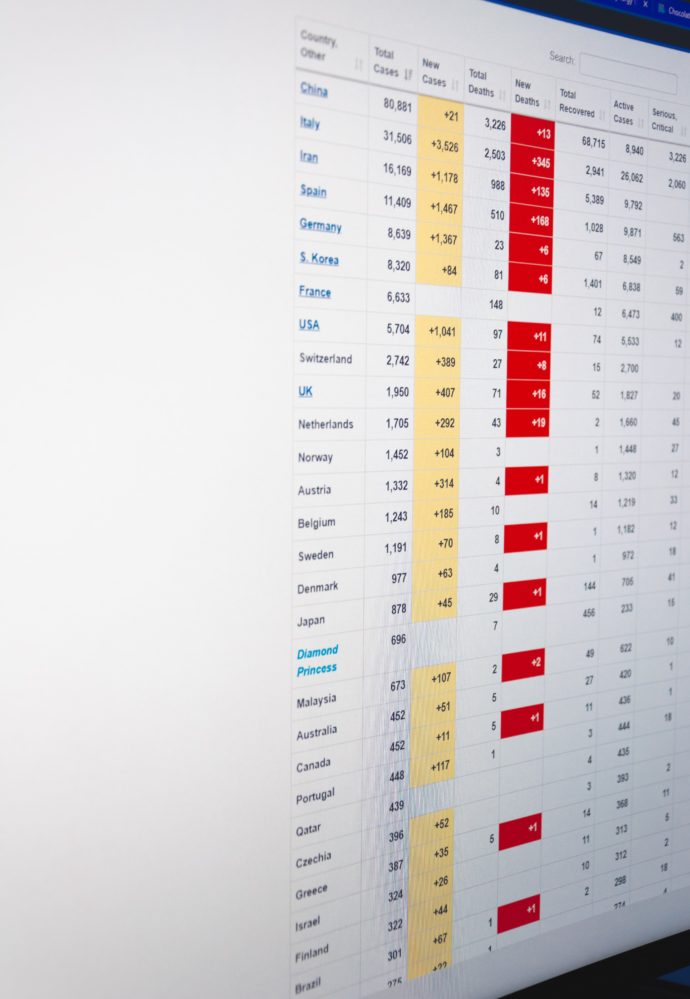
For the third week in a row, new COVID-19 cases have topped 300,000 (nearly 1 million in total) while the number of new deaths remains relatively low and stable (12,000 in sum over the past three weeks) according to the CDC’s cases in the U.S. website which the FEHBlog tracks.
Axios echos the FEHBlog’s sentiment that the medical profession to its credit has learned how to treat COVID-19. That is what you would expect in 2020. Hopefully the government is doing a good job providing healthcare resources to hot spot areas in order to facilitate treatment. In that regard, HHS announced today that “it will begin distributing $10 billion in a second round of high impact COVID-19 area funding to hospitals starting next week.”
In our FEHBP world —
- Federal News Network reports that OPM has issued new proposed rules to address enrollment problems that arose during the long government shutdown in the winter of 2018-19. Hopefully we won’t encounter another one of those unfortunate events again, but it is better to be safe than sorry. Several of the new flexibilities are already law thanks to a law that Congress passed in 2019.
- OPM also released today a revised SF 2809 FEHB enrollment form. The form is a handy reference for FEHB enrollment rules. It’s not used as often as it was pre-internet and smart phones.
Finally, the Trump Administration enjoyed two victories in the U.S. Court of Appeals for the D.C. Circuit today. As Healthcare Dive reports
- The Court of Appeals affirmed a lower court decision upholding the Administration’s short term duration health plan rule. The FEHBlog sees no harm in giving consumers greater choice of health care coverage after Congress zeroed out the individual mandate.
- The Court of Appeals reversed a lower court decision and thereby upheld the Administration’s Medicare “site neutrality” rule that “reduced some payments to off-campus hospital outpatient departments to make them consistent with other outpatient payments.” The court reasoned that
“Reducing the payment rate for a particular OPPS service readily qualifies, in common parlance, as a ‘method for controlling unnecessary increases in the volume’ of that service,” according to the opinion. “The lower the reimbursement rate for a service, the less the incentive to provide it, all else being equal. Reducing the reimbursement rate thus is naturally suited to addressing unnecessary increases in the overall volume of a service provided by hospitals.”
Makes perfect sense to the FEHBlog.