Thursday Miscellany

From Capitol Hill, Healthcare Dive reports
A group of 375 organizations sent a letter to the Senate on Tuesday urging lawmakers to act to pass legislation extending COVID-19-era telehealth flexibilities for another two years.
The letter was led by health IT and telehealth lobbies, but also joined by a number of health systems including Ascension and Cleveland Clinic, physician groups including the American Medical Association, tech companies including Amazon and Google and large employers including Walmart.
Without action, the policies — which threw open the doors to telehealth and led to skyrocketing utilization in the early days of the pandemic — will expire 151 days after the end of the COVID-19 public health emergency.
Health Payer Intelligence adds that according to a recently conducted survey on consumers enrolled in employer-sponsored health plans commissioned by AHIP:
First, most consumers across the political spectrum agreed that providers should not be permitted to charge unnecessary administrative fees and medical services mark-ups. Nearly eight out of ten respondents said that they supported this statement (78 percent), with three-quarters or more in each political party reporting this response.
Second, there was also strong bipartisan support for protections against hospital monopolies. Over three-quarters of consumers supported preventing hospitals from consolidation, mergers, and acquisitions that involved bringing other medical practices into one hospital system (76 percent). Consumers also indicated support for protections against site-based cost increases (75 percent).
Respondents wanted more transparency about healthcare deals. Slightly more than seven in ten consumers supported improving transparency around private-equity firms’ healthcare acquisitions.
Third, the researchers also found bipartisan alignment around telehealth. Slightly more than two-thirds of respondents agreed that the government should eliminate regulatory barriers to telehealth utilization (67 percent).
“Consumers value choice and flexibility in how they access health care. Telehealth proved to be an essential resource for consumers throughout the COVID-19 pandemic and should continue to play a role in the future of health care,” the survey stated.
To provide context, Beckers Hospital CFO Report informs us
HHS is set to extend the COVID-19 public health emergency [PHE] by its standing deadline of Oct. 13.
HHS last renewed the PHE July 15 for another increment of 90 days with a pledge to provide states with 60 days’ notice if it decided to terminate the declaration or allow it to expire. Aug. 14, the date in which states would have 60 days’ notice, came and went without updates or notifications from the agency, suggesting the declaration will extend.
If renewed on the deadline of Oct. 13, the next deadline would be Jan. 11, 2023. * * *
For an overview of the flexibilities tied to the PHE and what occurs when the declaration ends, check out a comprehensive brief from Kaiser Family Foundation here.
In No Surprises Act news yesterday, the NSA regulators issued a request for information (RFI) from stakeholders and the general public. The RFI concerns the law’s requirement that health plans provide an advance explanation of benefits (AEOB) in response to a good faith estimate (GFE) of healthcare costs requested by the patient to their healthcare provider. The provider would submit the GFE request to the health plan. HIPAA governs many similar claims transactions involving providers and payers. Surprisingly, Congress did not add these claim transactions to HIPAA, which would have made perfect sense. The FEHBlog does not understand why the regulators have not asked Congress to take this necessary step. At first glance, the contemplated process strikes the FEHBlog as unnecessarily complicated if the object is to avoid patient surprises. Nevertheless, at least the regulators are seeking public input.
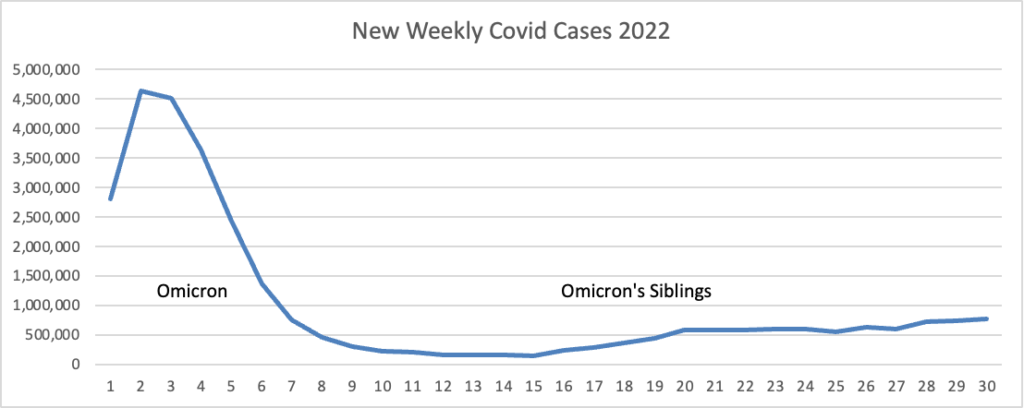
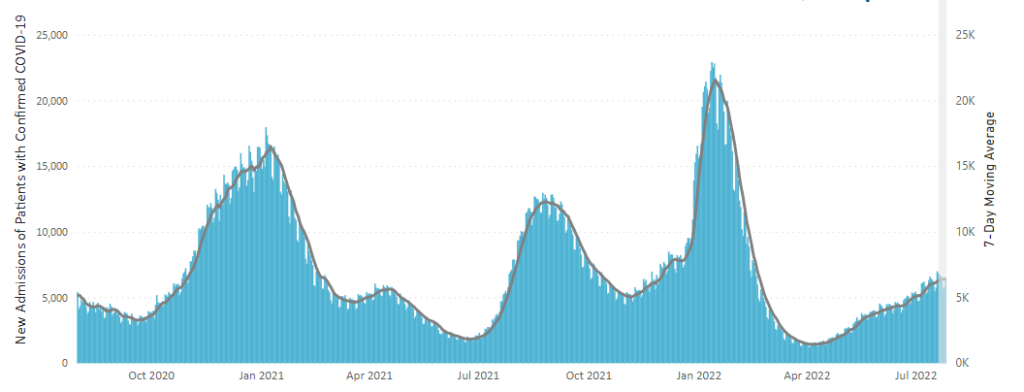
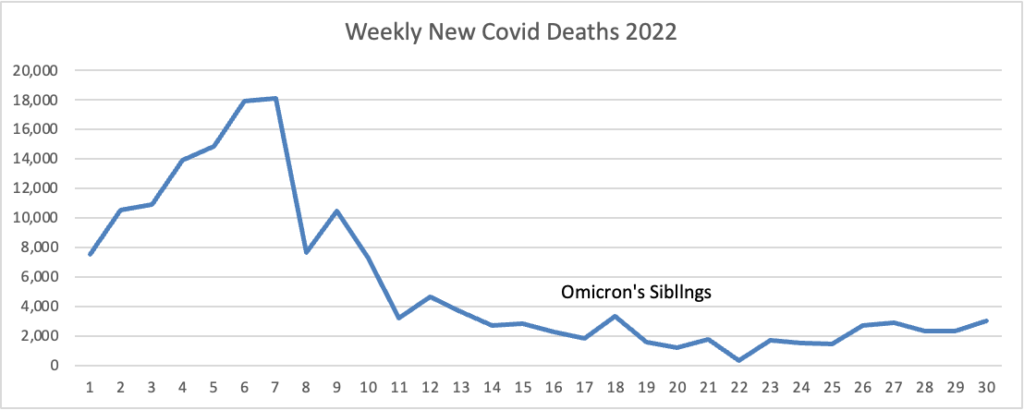
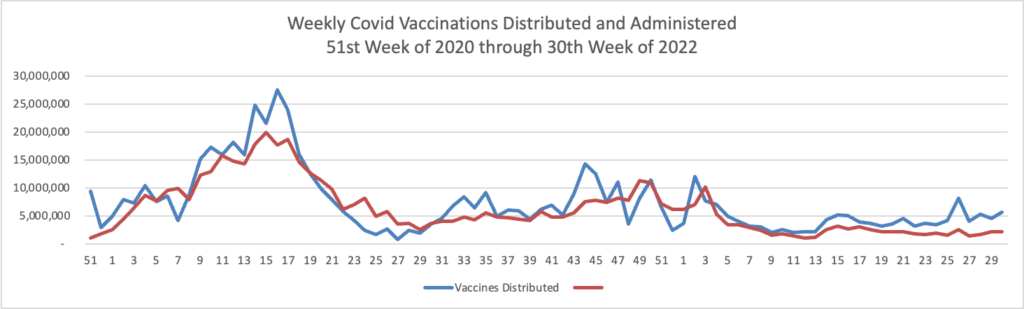
From the Omicron and siblings front, the National Institutes of Health announced
A research team funded by the National Institutes of Health has shown that commercially available rapid antigen tests can detect past and present variants of concern and has identified potential mutations that may impact test performance in the future. As new variants of the SARS-CoV-2 virus continue to emerge, concerns have been raised about the performance of rapid antigen tests.
The team, which was funded by NIH’s Rapid Acceleration of Diagnostics (RADx®) Tech program, developed a method to evaluate how mutations to SARS-CoV-2 can affect recognition by antibodies used in rapid antigen tests. Since most rapid antigen tests detect the SARS-CoV-2 nucleocapsid protein, or N protein, the team directly measured how mutations to the N protein impacted diagnostic antibodies’ ability to recognize their target.
“Rapid antigen tests remain an important COVID-19 mitigation tool, and it is essential to ensure that these tests can detect the SARS-CoV-2 virus as it continues to evolve,” said Bruce J. Tromberg, Ph.D., director of the National Institute of Biomedical Imaging and Bioengineering (NIBIB) and lead for the RADx Tech program at the NIH. “Considering the endless cycle of new variants, the data from this study will be useful for years to come.”
From the healthcare technology front, Fierce Healthcare informs us
[Cigna’s] Evernorth is expanding its digital health formulary yet again, adding five new solutions to the platform.
The formulary will now include Big Health’s Sleepio for insomnia and the tech company’s Daylight tool for anxiety. In addition, Evernorth said it will expand inclusion of Quit Genius’ tools to its platforms for alcohol use disorder and opioid use disorder.
Lastly, Evernorth will now include HealthBeacon’s Injectable Care Management System for inflammatory conditions, which is meant to assist patients in managing injectable medications. Glen Stettin, M.D., chief innovation officer at Evernorth, told Fierce Healthcare that all of the new tools fit key concerns for employers and plan sponsors, such as mental health and high-cost inflammatory conditions.
“Our clients care about areas where either lots of people need help and treatment or where they’re spending lots of money,” Stettin said.
From the federal employee benefits front, benefits expert Tammy Flanagan writing in Govexec discusses how federal employees should time their retirement.