Tuesday Tidbits
The Senate Health Education Labor and Pensions Committee held a COVID-19 hearing today featuring a number of federal government healthcare luminaries including Dr. Fauci. Here is a link to the hearing and the submitted testimony. The Wall Street Journal reports
Dr. Fauci said that with some states reopening before seeing a steady decline in cases and deaths, “there is a real risk you could trigger an outbreak…that could set you back rather than going forward.”
Adm. Brett Giroir, who is heading up the administration’s testing efforts, said an increased focus on testing in schools could be used as a means of surveillance to help ensuree students stay healthy.
Other health officials also emphasized the need for widespread testing to get a more accurate picture of how many people have fallen sick and to spot potentially undetected clusters of cases.
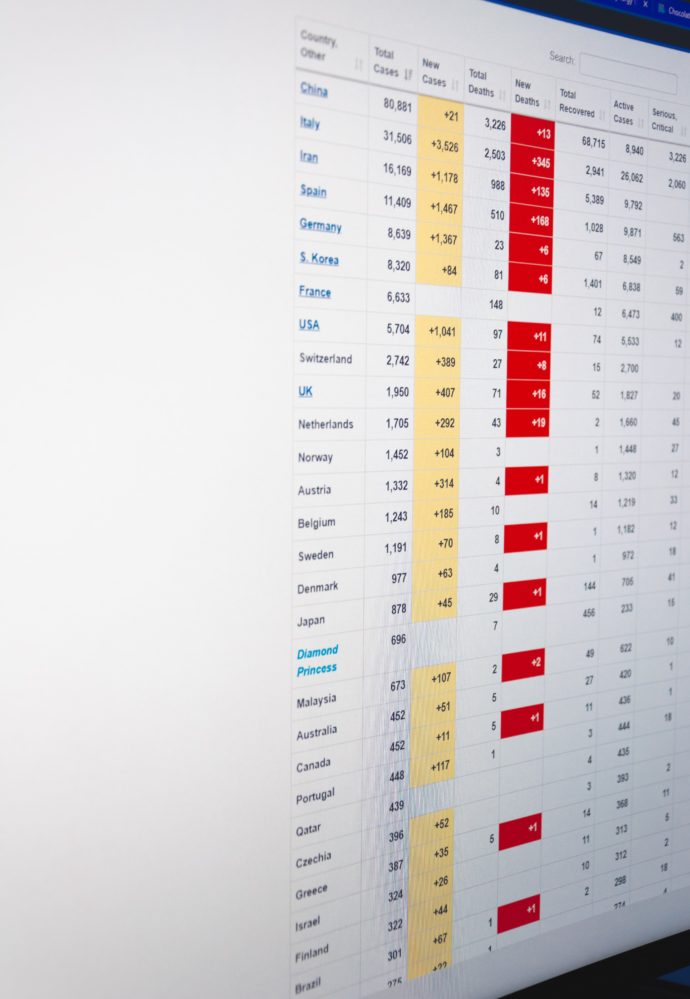
Here’s a link to the COVID Tracking Project site which provides a ton of state by state COVID-19 data, including testing data. As previously noted, GoodRx offers a complete, growing list of drive up COVID-19 test sites. Last week, one of the big U.S. lab test companies, LabCorp, began to offer “expanded access to COVID-19 antibody test through LabCorp’s wide network of doctors, healthcare providers, and online. Individuals have the ability to receive the COVID-19 IgG antibody test from their doctor, in person or through a telemedicine program, and now directly using www.LabCorp.com/antibody-testing.“
A friend of the FEHBlog pointed out this National Institutes of Health website which is chock-a-block full of COVID-19 research tidbits. For example, the FEHBlog noticed a NIH study finding “nearly everyone who recovers from COVID-19 makes coronavirus antibodies.” Check it out.
The Hill brings us to date on the four leading U.S. and European COVID-19 vaccine development efforts. “There are more than 100 potential vaccine candidates, according to the World Health Organization, but only eight have entered the crucial clinical trials stage. Four are in the United States and Europe, with the rest in China.”
Healthcare Dive reports that the American Hospital Association flipped out over new price transparency rules in the fiscal year 2021 Medicare Part A hospital PPS changes proposed rule released yesterday.